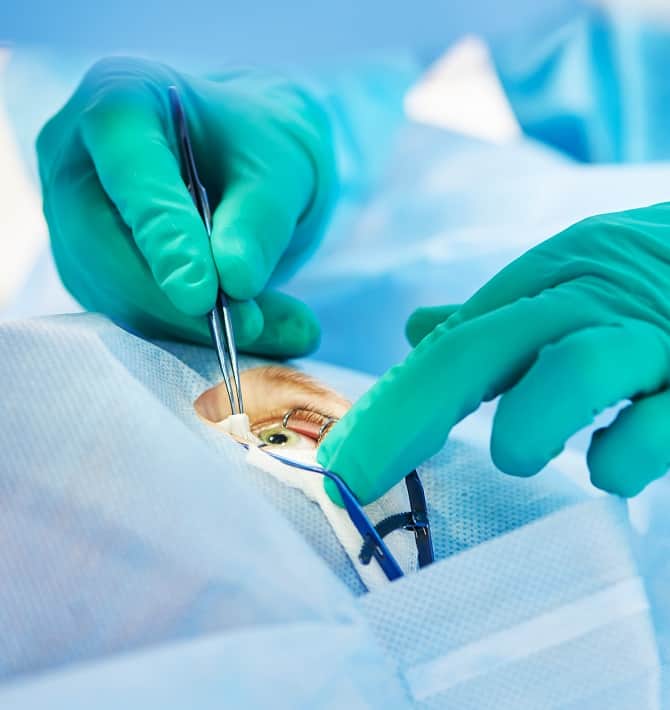
Austin TX Corneal Transplant Surgery
We have been doing DSAEK and DSEK since early 2008. The results have proven themselves to be much better than the results of full-thickness cornea transplantation. There is recovery of functional vision within weeks (rather than 6-12 months with full-thickness cornea transplantation), the procedure is safer and less invasive than regular cornea transplantation.
Advantages of DSEK (over full thickness Corneal transplantation aka Penetrating Keratoplasty/PKP):
- Stronger wound, resistant to trauma.
- Corneal nerves preserved.
- Faster recovery of vision compared to full-thickness cornea transplantion.
- No suture related complications.
DMEK or Descemet’s Membrane Endothelial keratoplasty represents the most advanced form of lamellar keratoplasty for treatment of Fuch’s dystrophy, Pseudophakic bullous keratopathy and corneal clouding from corneal endothelial dysfuntion. Austin Eye began is proud to be one of the few centers in Texas to offer DMEK for our patients.
Advantages of DMEK (over DSEK):
- Lowest rejection rate, smallest incision, best visual potential of any corneal transplant surgery
- Less induction of refractive errors/hyperopic shift
About Austin Eye
For those seeking an experienced eye doctor Austin residents trust, Austin Eye features a team of highly qualified Austin eye care providers dedicated to providing patients with a top-quality vision correction experience. The surgeons at Austin Eye have many years of experience and training in a variety of eye surgery procedures.
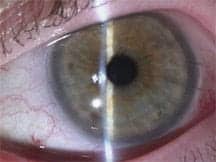
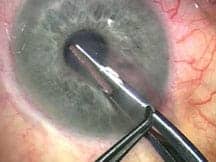


The Mitchel and Shannon Wong Eye Institute

The Mitchel and Shannon Wong Eye Institute, recently created at the Dell Medical School, is poised to become a leading-edge center for training future ophthalmologists and providing patients with the best medical and surgical eye care possible.
Contact Austin Eye Today

11901 Jollyville Road
Austin, TX 78759
Phone: (512) 250-2020
Fax: (512) 250-2612
Click here to “FLY-through” our Northwest Office
Office Hours
Monday – Thursday 8am – 6pm
Friday 8am – Noon
Saturday/Sunday Closed

2700 Bee Caves Road
Austin, TX 78746
Phone: (512) 250-2020
Fax: (512) 250-2612
Click here to “FLY-through” our Westlake Office
Office Hours
Monday – Thursday 8am – 6pm
Friday 8am – Noon
Saturday/Sunday Closed